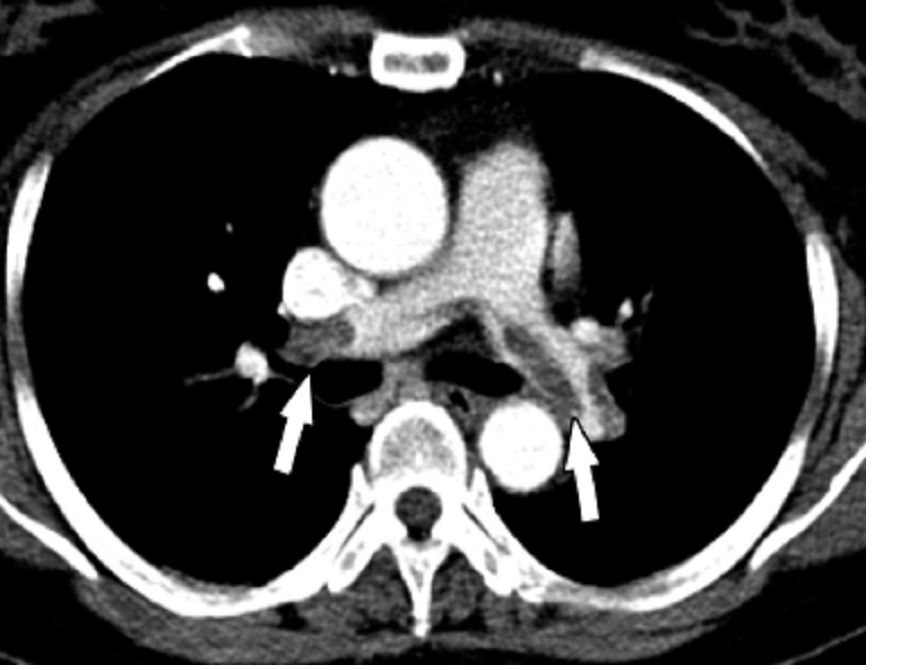
When it comes to conditions that pose a sudden risk to one’s health, pulmonary embolisms do not share the same level of awareness that heart attacks or strokes do.
However, this condition is a deadly one, as it is responsible for as many as 200,000 deaths in the United States alone. In this article, we will discuss what a pulmonary embolism is, the signs and symptoms it poses, how it is treated, and whether you might be at risk for developing one later in life.
What is a pulmonary embolism?
A pulmonary embolism is a blockage of an artery in the lung that is caused by an obstruction that has traveled there from elsewhere in the body.
Most often, this is caused by a blood clot that has broken up in a vein or artery in the patient’s legs or arms. A lack of blood to the lungs poses serious problems for respiration and more dangerously, it begins the process of tissue death in the affected lung.
How do I know if I might be having a pulmonary embolism?
The prognosis for surviving a pulmonary embolism if caught early is good, as fewer than 10% of fatal PE cases occur in the first hour of the event.
If you find yourself short of breath and attempting to make up the shortfall by breathing rapidly, suffering chest pain, and/or coughing up blood, you are probably suffering a pulmonary embolism.
If you or a loved one has blue fingertips or lips, or you have collapsed suddenly, you are entering the latter stages of this condition, and you need to get to an emergency room immediately. In either case, being admitted to a hospital is key to surviving the next several hours.
How are pulmonary embolisms treated?
Once you have arrived at the emergency department of your local hospital, they will wheel you in for immediate treatment. In order to resolve a pulmonary embolism, the attending physician and their nurses will undertake a variety of treatments depending on the severity of the case.
In its early stages, doctors may administer anticoagulant drugs such as heparin and warfarin to thin the blood and help break up the blockage in a non-invasive manner.
In more recent times, doctor has gained access to machines like the EKOSonic, which uses ultrasound waves to add another vector of attack alongside the injection of anticoagulants to help break up clots more effectively.
Finally, some doctors opt for surgical intervention, although the higher risk involved in this invasive maneuver make it an option of last resort for emergency care providers.
Am I at risk?
While it is possible for anyone to develop internal blood clots, there are certain lifestyle choices that make it more likely for certain segments of the population.
If you have a family history of blood clots, currently have heart disease or cancer, or have had surgery recently, you are at a heightened risk for developing blood clots, and therefore, have a higher risk of suffering a pulmonary embolism.